Knee Replacement
Knee Replacement Resource Hub
Search our comprehensive knee replacement guide for answers on surgery, recovery, and daily life.
Quick Facts
Everything You Need to Know
Don’t let a worn-out knee limit your independence.
Schedule a consultation to discuss your personalised surgical plan.
Diagnosis
Identifying the source of your discomfort. Learn how we use weight-bearing X-rays and clinical evaluations to determine if a knee replacement is the right solution for your mobility goals.
Osteoarthritis of The Knee
What is OA?
Osteoarthritis or wear and tear of the knee typically occurs in old age. It is characterized by a general wear and tear of the knee. In addition to the thinning and disappearance of the cartilage, the quality of the meniscus also deteriorates with age. As a result, these structures lose their shock-absorbing function, which leads to overloading of the underlying bone.

Symptoms
The complaints consist of a typical mechanical, load-related pain. Swelling, warmth and stiffness can also occur. All this leads to a loss of function, such as being unable to walk far, difficulty rising from a chair, or climbing stairs. Initially, the complaints are variable, good days and bad days are experienced. In the long term, the complaints will become more pronounced. In some cases varus(bowed) or valgus(x-Legs) deformations of the knee can occur.
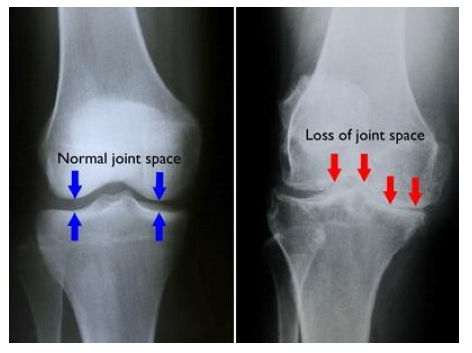
Diagnosis
An important examination in osteoarthritis are the Xrays. These are best performed while the patient is standing so that the narrowing of the joint can be properly appreciated. An MRI scan might be indicated in cases where expected cartilage damage is present.
Treatment
Treatment initially consists of symptom control with painkillers and anti-inflammatories. Muscle strengthening and adjustment of the load are also advised, this is important in old age. A brace can also help. In Patients with an increased BMI, a reduction of 10% can offer a lot of improvement. Finally, injections can also be administered in the knee, either with a gel or with a powerful anti-inflammatory. If conservative treatment fails, the next step is surgery. In the case of advanced degeneration, the option of a knee replacement can be discussed with the patient. In less pronounced forms of wear, other options such as an arthroscopy or an osteotomy can be considered.
Procedure
Where expertise meets innovation. Discover how Mako™ SmartRobotics provides a level of precision tailored specifically to your anatomy, ensuring a more natural-feeling joint.
Knee Replacement
What Is A Knee Replacement?
To understand what a total knee replacement is, you first need to understand what a normal knee joint looks like. This joint is composed of three parts that are covered with cartilage.
- The upper part (the bottom of the femur) consists of two spherical heads resting on the tibia
- The lower part consists of an almost flat surface of the tibia
- The kneecap (patella) is embedded in the large thigh muscle and also forms a joint with the thigh bone(femur).
Those three parts are covered with the cartilage that serves as a sliding layer and ensures that the knee can move smoothly. In addition, there are the meniscus that serve as shock absorbers and the ligaments and cruciate ligaments that provide stability.
Why A Knee Replacement?
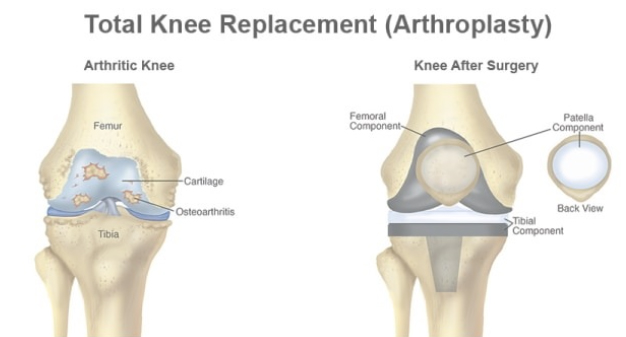
A knee prosthesis is the definitive treatment for osteoarthritis of the knee. Knee osteoarthritis means the wearing away of the smooth cartilage layer in the joint. As a result, the joint surfaces can no longer slide smoothly over each other, and moving becomes increasingly difficult and painful. A full knee replacement is an artificial joint that replaces the damaged cartilage of the knee joint.
Because the knee joint consists of three different parts, a knee prosthesis usually also has three separate parts: an upper leg component, a lower leg component, and a kneecap component(figure 1). In principle, there is no age limit and both younger and older patients are eligible. Modern prostheses last an average of fifteen to twenty years. After that period, if the prosthesis shows wear or begins to loosen, it can be replaced. It used to be said that only 1 replacement was possible. With today’s techniques, multiple replacements are possible. You may expect that a large part – if not all – of your osteoarthritis pain has disappeared, or has become much less. The mobility of the joint remains about the same as before the operation. How flexible the knee becomes after surgery is strongly determined by how much and how well you exercise afterwards. As soon as you have healed after placing your prosthesis, you can walk again, cycle and swim. If your rehabilitation goes well, you may do sports to a limited extent, such as playing tennis and golf.
Types Of Knee Replacements
Total Knee Replacement
The knee replacement is the ultimate treatment for osteoarthritis. A knee prosthesis is a very good treatment for severe wear and tear of the knee and insufficient improvement of the complaints with pain medication.
The long-term results with the current implants (knee prosthesis) show a survival of 95% at 10 years and 85% at 20 years. Most patients can therefore continue with their knee prosthesis for the rest of their lives. There are different types of knee arthroplasties: total knee arthroplasty, unicondylar knee arthroplasty (or half knee arthroplasty) and patellofemoral knee arthroplasty (or kneecap arthroplasty).
The full or total knee arthroplasty is the most frequently performed knee arthroplasty. This is used when the entire knee is worn out. During the procedure, the damaged cartilage is removed and replaced with a new metal covering about 9 mm thick. This knee prosthesis is attached to the femur and tibia with a kind of bone glue or cement. Between the 2 metal components is a plastic component made of very hard and wear-resistant polyethylene over which the knee can flex and stretch smoothly.
All this is done using a muscle-sparing technique that speeds up rehabilitation after knee replacement surgery. By placing the knee prosthesis, the activity-related pain disappears and the mobility of the knee improves. After rehabilitation, the knee should be able to bend smoothly. Fully straightening the knee is also very important. You may or must be active with a knee prosthesis: walking, cycling, swimming, fitness are all no problem. However, contact sports are not recommended.
After the operation, the patient usually stays in the hospital for 3-5 days, followed by 6 weeks of rehabilitation with physiotherapy.
Unicompartemental knee replacement
The half knee prosthesis or the unicompartemental knee replacement is placed when only part of the knee is worn (inside or outside). So not everyone qualifies for this. The big advantage of this type of knee prosthesis is that a large part of your own knee, including the cruciate ligaments, can be preserved. For patients, this means faster rehabilitation and a knee that feels more stable and more natural. Also in the long term, the half knee prosthesis has proven to last at least as long as the total knee prosthesis. A half knee prosthesis is also a valid option in the elderly if the indications are correct.
Patellofemoral Joint Resurfacing
The patellofemoral prosthesis or the kneecap prosthesis is a kind of half knee prosthesis for people with isolated wear to the patellofemoral joint. The advantages are the same as for the half knee prosthesis: a large part of your own knee, including the tibiofemoral joint and the cruciate ligaments can be preserved.
Robotic-Assisted Total Knee Replacement
By switching on the robot, the position of the knee prosthesis can be individually adjusted to the specific anatomy and biomechanics of the patient. The Mako helps the surgeon determine the optimal position of the knee prosthesis tailored to each individual patient. After this calculation, the Mako helps to carry out this plan by also implanting the knee prosthesis extremely accurately. This type of cutting-edge technology is accurate, reproducible and delivers superior results.
During the operation, the knee robot not only helps to make bony sections, but based on artificial intelligence, the Mako robot also provides the surgeon with important additional information. First, providing the surgeon with additional information about the specific anatomy and biomechanics of the specific patient.
In this way, the most optimal position of the knee prosthesis can be determined in advance for each individual patient. Once the optimal position of the knee prosthesis has been determined, the robot then helps to execute the plan via a robot-controlled arm, making very precise bony sections up to 0.5 mm accuracy.
With the robot, we as surgeons can now plan the procedure very accurately and also achieve the outcome effectively. Another advantage of the robot is that the tissues are spared as much as possible during sawing. As soon as the saw blade comes out of the bone, the saw motor stops; this is called haptic feedback.
In this way, the surgical trauma is further reduced, which ensures a smooth and rapid rehabilitation. This minimizes the risk of complications. Robots have been used in the operating theater for some time. A high-quality Robot, software integration, CT scans and a multidisciplinary team are all part of making this possible.
The future is upon us and with assisted accuracy and reproducibility, I am truly convinced that robotic surgery is the future.
Revision Knee Prosthesis
A revision knee prosthesis is an operation in which a previously placed knee prosthesis that is worn, does not work properly or has become loose, is replaced again. Before deciding on a revision operation, it is always important to thoroughly investigate the cause of the problem. For this, the doctor will prick the knee to examine the fluid and perform some additional imaging.
A revision procedure is truly tailor-made in which the specific problems are addressed. And this can be different for every patient. Depending on the problem, the previously installed parts are removed in whole or in part and replaced by new ones. The revision prosthesis is usually fitted with stems for better anchoring in the bone. A revision operation is a more difficult operation than a first knee replacement and usually also requires a longer rehabilitation.
Surgery
The Operation
Before the procedure, you will be thoroughly checked in all areas so that the procedure can be optimally performed. In addition, there are a number of other matters such as physiotherapy, home care and possibly a rehabilitation center that are best arranged in advance.
Important
Tell your specialist if you are taking blood thinning medicines. He will tell you when to stop taking these before surgery.
The operation itself takes an average of one to two hours. You will receive more information about the course of the operation itself at the information session. Afterwards your knee is wrapped in a thick bandage. After the operation you will be taken to the recovery room, also called recovery. There you will be under the supervision of an anesthesiologist and a nurse for several hours. Your blood pressure, pulse, temperature and pain are systematically monitored. The blood circulation and the mobility of your leg are checked. It is therefore important to report a feeling of numbness and/or pain in the leg or foot to the nurse.
When your blood pressure and heart rate are stable, you will return to the ward.
It will often take at least 4 to 5 hours after surgery before you are taken back to the ward. It is best to inform your possible visitors that you will not be back in your room until the late afternoon or early evening. After the operation, a large compressive and absorbent bandage is applied. When you are back in your room, the nurses on the ward will take over the care. You may start drinking water a few hours after the operation. You may receive a light meal in the evening. The IV will remain in your arm until the next day to administer fluids, antibiotics and pain medication.
Medication
You will be given antibiotics during the operation to minimize the risk of infection. Your doctor will also prescribe blood-thinning medication to prevent thrombosis (= clotting of the blood). You will be given this blood-thinning medication every day until about 4 weeks after surgery.
You will be given a schedule of the pain medication you can take. For the first few days you will be given pain medication to take home and you will also receive a prescription. It is important that you take pain medication regularly during the first few days. The medicines not only relieve pain, but they are also good for reducing swelling.
Risks & Safety Protocols
Complications
We do everything we can to avoid complications and in most cases an operation goes without problems. Nevertheless, it is important that you know which complications can occur.
Infections
Many preventive measures are taken in the operating room to prevent infections. You will also be given a short course of antibiotics.
Thrombosis, possibly pulmonary embolism
For this you will receive preventive anticoagulants that must be administered as prescribed. Doing plenty of calf pump exercises is also important. The physiotherapist will teach you this.
Nerve injury
Limited mobility
It is very important to bend the knee more than 90° within the first ten days.
Warning signs
Complications are usually very limited. They often mean only a delay in rehabilitation. It is important to inform your surgeon in good time if one of the following warning signs should occur:
- if pain in the surgical area increases in combination with discharge, redness or fever .
- If the knee becomes increasingly difficult to move and more painful when exercising.
- If you are short of breath and/or have pain in the chest area
- If you have swelling of the leg/calve with warmth,redness and increasing pain.
Symptoms of possible complications
Call your general practitioner, the orthopedics surgeon or the emergency department. If any of these symptoms occur
- fever of 38.5°C or higher
- abnormal redness, warmth, or discharge from the wound
- a lot of pain in the knee that is not relieved by painkillers
- pain or swelling of the calf
- tingling or difficulty moving the foot and toes
- decreased appetite or general malaise
If you inform the surgeon in time, he can quickly take the appropriate measures to treat these complications.
Prep & Recovery
The roadmap to your new life. What to expect from your hospital stay, how to prepare your home, and the milestones of your rehabilitation journey.
Hospital Stay
What To Bring To Hospital
In addition to the usual things such as nightwear and toiletries, you can also bring:
- medicines that you already use at home
- comfortable clothing that allows you to free your upper leg
- your identity card
- comfortable shoes that you wear during the day. They must be tight on the foot and have a wide heel (no slippers). Tightly closed shoes are necessary.
- Two crutches: you can rent these from hospital or buy your own
Important Information
Make sure you are fasting before the procedure. This means that you are not allowed to eat or drink anything (including water) from midnight on the night before the operation.
Take a bath or shower at home the morning before the operation, so that the procedure can take place in the most hygienic conditions. Make sure you report to the hospital at the appointed time.
You will take the following items home:
- The date for a check-up appointment with your surgeon.
- The necessary pain medication.
- A letter with your rehabilitation program and a prescription for your physiotherapist.
The doctor will monitor the use of blood thinners when you return home. You will receive further physiotherapeutic guidance at home
Day of Surgery
You will be put on a surgical gown and a nurse will take you from the ward to the preparation area of the operating theater in your bed. An IV is inserted in the operating room. The anesthesiologist will then start anesthesia. If you have any questions about this, you can ask the anesthesiologist, the week before the operation at the preoperative screening session.
After the Operation
Hospital Recovery
Day 1
On the first day you will be guided in the first steps with a walking frame. You may put full weight on your operated knee. Your physiotherapist and occupational therapist will help you in a comfortable chair, which you can put in a relaxing position.
Day 2
From now on you will go to therapy on the ward in normal clothing in the morning and afternoon. You will receive the exercises in an exercise room under the supervision of an experienced physiotherapist and occupational therapist.
Day 3
From the third day you can already go up and down a flight of stairs with crutches. Your physiotherapist is present daily during the exercise sessions. He or she will teach you the best method to safely resume your daily activities independently. You can go home from the 3rd day after the operation.
Visiting hours
Try to limit your visit. You could still use a rest break. The exercises take place twice a day. It goes without saying that your partner or coach can come by at any time of the day. You may return home once your medical treatment has ended. The average length of stay in hospital is usually about 3 days, but depends on the healing of your wound, general recovery and rehabilitation.
At Home Recovery
It is best to inform your home physiotherapist about the procedure so that he can guide you when you return home after the operation/ knee replacement. You can also make an appointment with the home nurse for wound care and postoperative medication (if needed).
Exercise at home
As soon as you return home, the rehabilitation will continue under the supervision of your physiotherapist. Mobility will be increased step by step and the use of crutches will be reduced. You can cycle again as soon as the knee can bend sufficiently. Sports and other hobbies are possible provided that the knee is not overloaded. Always discuss this with your physiotherapist, your general practitioner or your surgeon. The more you exercise at home, the faster you will progress in agility and strength. The exercise program will be gradually expanded by your home physiotherapist. He /she will tell you more about this when you return home.
Exercise schedule
This schedule is intended to help you remember the exercises that the physiotherapist has discussed with you. There are exercises that are mainly intended for the first days after surgery and exercises for a little later. It is not the intention that you start new exercises on your own initiative, unless after consultation with your physiotherapist. You will be taught the first bending and stretching exercises after surgery in various ways. You may find it difficult to tighten your front thigh muscle. That is why you also get trained every day to stimulate the muscles.
- In general, you exercise almost every hour during the first few days and this is reduced to two to three times a day in a later phase. At first you may feel some stretching, pain and some fatigue. It is important to never exaggerate and fast track the exercises.
- Initially it is important that you can walk again with an aid (crutches). In case of severe pain and/or swelling, you should take some rest. If necessary, take it easy for a day.
- It is also important that you take deep breaths in and out regularly and calmly on the day of the operation and the day after. In this way you stimulate your breathing during the period in which you mainly lie or sit.
Important
- Two weeks after the operation/ knee replacement you should be able to bend your knee 90°. If not, please contact your doctor.
- Each exercise may be repeated five to ten times, within the pain threshold. Avoid exercises that are too difficult or painful.
FAQ
Clear answers for a confident journey. We address the most common patient questions regarding lifestyle, safety, and long-term results.
How is the surgical wound treated?
There are several ways to close the surgical wound: with hooks, thread or subcutaneous suture with 2 loops at the ends of the wound. The wound should be kept dry and clean for 14 days. The bandage certainly does not need to be changed daily. If there are blisters, red edges or a discharge, inform the nurse. He/she can assess the wound and recommend early consultation with your surgeon if necessary.
Do I have to go on a diet or is special food recommended?
No, there are no dietary restrictions. Back in the room, in consultation with the head nurse and the doctor, it will be decided when you can eat normally again. You will usually have a light meal in the evening after the operation and you can usually have a normal meal the day after the operation. Keep in mind that some painkillers can suppress appetite or cause nausea.
Can I drive?
For safety reasons, it is best not to drive a car yourself until after the check-up with your doctor, which is usually six weeks after the procedure. After all, you must always be able to perform an emergency stop by law. This measure is therefore not intended to take away your freedom, but rather to protect you.
Is travel allowed?
It is best to wait until about six weeks after the procedure. Keep in mind that some aids such as crutches or walking sticks are still necessary.
What about sexual activity?
Sexual activity is possible as soon as you feel capable. Your physiotherapist or your doctor can answer any questions about this.
Activities?
There are exercises that are mainly intended for the first days after surgery and exercises for later, when you are back home. You are not supposed to start new exercises on your own initiative. You can discuss this with your physiotherapist. You may find it difficult to tighten your front thigh muscle. That is why a muscle stimulus is administered every day to help you strengthen this muscle. In general, you practice almost every hour during the first days and this is reduced to two to three times a day in a later phase. You may feel some stretch while exercising and you may experience some fatigue. However, never exaggerate. In the first place, it is important that you can walk back with an aid (walking frame or crutches). Do this as often as pain and fatigue allow. In case of severe pain and/or swelling, you should take some rest. You can then also place some ice in the groin and against the side of the leg. If necessary, take it easy for a day. It is also important that you take regular, deep breaths in and out on the day of surgery and the day after. In this way you stimulate your breathing during the period in which you are mainly lying or sitting. Each exercise may be repeated five to ten times, within the pain threshold. Avoid exercises that are too difficult or too painful.
Life After Surgery
General Guidelines for a Knee Replacement
Life with a knee prosthesis is – certainly in the beginning – a change for you and your environment. It allows you to resume your normal daily activities and contacts.
Here we give you tips that can serve as a guideline for further good rehabilitation.
The ultimate goal after total knee replacement surgery is for the pain to go away and for you to regain your normal range of motion and strength. That is why you try to resume normal daily activities as soon as possible, such as walking, getting in and out of the bed, toilet, etc. It is wise to see any pain as a measure of the pressure you put on the knee. If the knee becomes sore, swollen, or warm, it could be a sign that you’ve been doing too much. Try to adjust both the load and your activities (how often you step, what distance) to this. If your knee or leg is swollen or hot, rest. Raise your leg. It is recommended to cool your knee with an ice pack several times a day. This promotes swelling and reduces pain. This ice pack treatment is followed consistently during your admission, but should of course be continued at home during the first 6 weeks.
Stairs
After the operation, you can immediately put full weight on the new knee. In the initial phase, this is sometimes difficult because of the wound pain. That is why you step with crutches in this initial phase.
You make sure you avoid the risk of falling;
- provide sufficient space to walk
- remove loose items (eg power cords and carpets)
- use an anti-slip mat in the shower
- On average, you will walk with crutches for about four to six weeks. Depending on the pain and swelling of your knee, this term may be revised by your physiotherapist
- For the first three weeks you will walk with two crutches. Both crutches move forward simultaneously, then the operated leg between the crutches and then the good leg in front of the crutches.
- From the fourth week you use one more crutch on the non-operated side. Then you place the crutch and the operated leg forward together.
When walking, always keep yourself upright and look ahead. When turning, always lift your feet and do not turn on the side of the operated leg.
Try to gradually increase your walking distance.
The correct height of the crutches is important. They are properly adjusted when you can support yourself with your hands on the handles and your elbows almost straight. It is also important to put caps with a sufficient profile under the crutches so that you do not slip.
To climb stairs
Take the stairs step by step. Both feet are next to each other on the same step before you start the next step. With one hand you take hold of the railing, on the other hand you hold both crutches.
Upwards
Support yourself firmly on both hands (crutch and handrail) and place the foot of the non-operated leg on the first step. Then add the crutch and the foot of the operated leg
Down
First, place the stool one step lower. Then place the foot of the operated side on the step where the crutch is. Then place the second foot next to the first.
Bed
Bed
It is important that your bed is high enough. If it is too low, it may make it difficult to get out of bed. Ideal is as the top edge of the mattress reaches above the back of the knee. If the bed is too low, you can temporarily solve this by placing blocks under the legs of the bed, laying a double mattress or getting a hospital bed at home (you can get these and other aids from your health insurance fund). Also a mattress that is too soft is not recommended. This will cause problems getting in and out of bed.
In bed
Sit on the edge of the bed just below the pillow. When sitting, place the operated leg a small step forward to avoid excessive bending of the knee when sitting. Push yourself up with both hands to sit further back until the knees are supported. Then rotate both legs and pelvis into the bed at once.
Out of bed
Sit up and lean on both hands. Rotate pelvis and legs together toward the edge of the bed. Slide further forward until you can support yourself with both feet on the floor. Then again place the operated leg a step forward and push off with both hands.
Possible aids for getting in and out:
- Hook the feet together, with the foot of the healthy side passing under the foot of the operated side
- Use a sling (e.g. large towel), place it under the foot of the operated side and lift the leg into bed with both hands
Sleeping
Sleeping on your back is no problem. It is important that your knee can be fully straightened. Therefore, do not lie with a thick pillow under the knee (see fig. 13). When you sleep on the right side, it is better to put a pillow between your knees, this will make it more comfortable for you.
Sitting and Rising From a Chair
Sit down
Avoid sitting in a chair that is too deep or too low. If necessary, place another cushion on the seat. If you want to sit down, step back towards the chair or seat until you can feel it with the backs of your legs. Before sitting down, put both crutches away or hold both crutches in one hand. Then lean on the railing with both or one hand. Place the operated leg one step forward to avoid excessive bending in the knee. Then sit down slowly.
To Get Up
Move to the edge of the seat. Make sure to move your operated leg slightly forward when standing up. Push off on the handrail (see fig. 14 and 15). Never try to get up by pushing up on both crutches as this is unstable and could cause you to fall.
Washing
During the first weeks you can take a shower, but only with a waterproof bandage. It is also not the intention to shower for too long as the skin starts to sweat and the bandage can come off. In and before the shower, you can use an anti-slip mat. Installing a support bar on the wall can also help if you lose your balance. Placing a plastic stool in the shower cubicle helps to avoid having to stand for long. There are also seats, folding chairs that are attached to the wall. It is best not to take a bath in the first six weeks because of the difficult movement in/out of the bath and to protect the wound. In the bath you can also use a bath seat, both foldable and hanging.
Toilet
If the toilet is too low and you have trouble sitting down or getting up from the toilet, a toilet seat raiser can be of great help. Installing a support bar on the wall helps with getting up. You can find these and other aids at your health insurance fund.
Dressing and Undressing
During the first weeks you may experience some difficulties in putting on and taking off clothing such as underpants, trousers, skirts, stockings and shoes. Try this while sitting and possibly place the foot on a chair in front of you (see fig. 17). Avoid squatting in the beginning. There are also a number of aids that can make the work easier. For example, you can use a stocking puller, a slip lift or a long shoe horn. Always wear sturdy shoes, so shoes with a heel piece or a strap to keep your heel in place. It is better not to wear slippers for the first few weeks to avoid falling.
Household
As long as you walk with crutches, it is best not to do major household tasks. As soon as you no longer need to use crutches, you can start gently, without forcing yourself. During the first weeks it is quite difficult to stand for a long time (e.g. when ironing, washing dishes or cutting vegetables). To do this, sit down and choose a high and stable stool. You should avoid much lifting in the first few weeks, especially as long as you are still using crutches (e.g. lifting a bucket, laundry basket). To pick up an object or to perform a task close to the ground, you should not squat for the first few weeks. It is best to proceed as follows: with the hand of the operated side, take a firm support (e.g. chair, table) and transfer your body weight to the non-operated leg. Bend the body forward and simultaneously swing the operated leg back. With your free hand you can now pick up the object without any problem
Gardening
Gardening is avoidable as long as you walk with crutches. Mowing the grass, for example, can only be carried out after six weeks. Whether you can still sit on both knees to work after the operation will depend on various factors (including pain sensitivity, flexibility). Therefore, it is not possible for everyone to do this even a long time after the procedure. If you sit on the knee to work, it is better not to do this on the operated leg (see fig. 20).
Walking
Walking is allowed during rehabilitation. Simultaneously increase the distance according to your condition. Always watch out for unevenness on the sidewalk and for curbs outdoors. Avoid bumpy, slippery or soft bottoms at first.
Cycling
You can start cycling on an exercise bike after three to four weeks, depending on the mobility of your knee. After about six to eight weeks you can start cycling outside again. Men should start with a women’s bike because of the low entry. Always do this in consultation with your orthopedic surgeon, general practitioner or physiotherapist.
Swimming
You can start swimming from the sixth week after surgery. This is a very healthy sport, but avoid excessive twisting movements when performing breaststroke.
Driving
If you have sufficient control over your operated leg, you can drive again after six weeks. Please check the conditions of your car insurance beforehand. If the car is too low, this can cause problems when getting out. In that case you can put a cushion in the seat to make it easier to get out of the car. Turntables are commercially available to improve the turning. You can also use two hard plastic bags. Placing them on top of each other makes it easier to turn in the car seat.
When getting in, put the seat back as far as possible.
You’ve explored the technology and the recovery path.
Now, let’s create a personalised surgical plan tailored to your lifestyle and goals.